Prescription Weight-Loss Treatments from UK Prescribers
Obesity is a chronic medical condition, not a lifestyle choice. As a prescribing clinician, I see patients who have tried every diet without lasting results because biology works against sustained calorie restriction. GLP-1 receptor agonists and other evidence-based medications now offer clinically significant weight loss of 10-15% when combined with behavioural support. Eligibility starts at BMI 30, or BMI 27 with comorbidities.
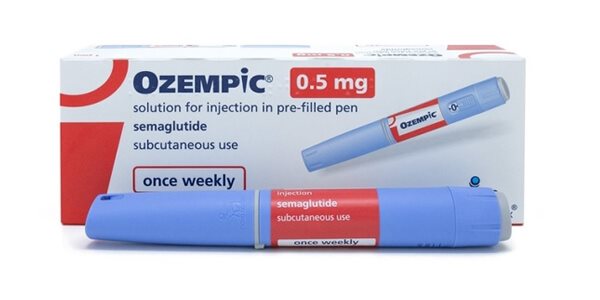
Semaglutide (Wegovy) produces mean weight loss of 14.9% over 68 weeks in the STEP 1 clinical trial
GLP-1 agonists reduce appetite by mimicking satiety hormones and slowing gastric emptying by 30-40%
NICE recommends pharmacotherapy when BMI exceeds 30 or 27 with weight-related comorbidities present
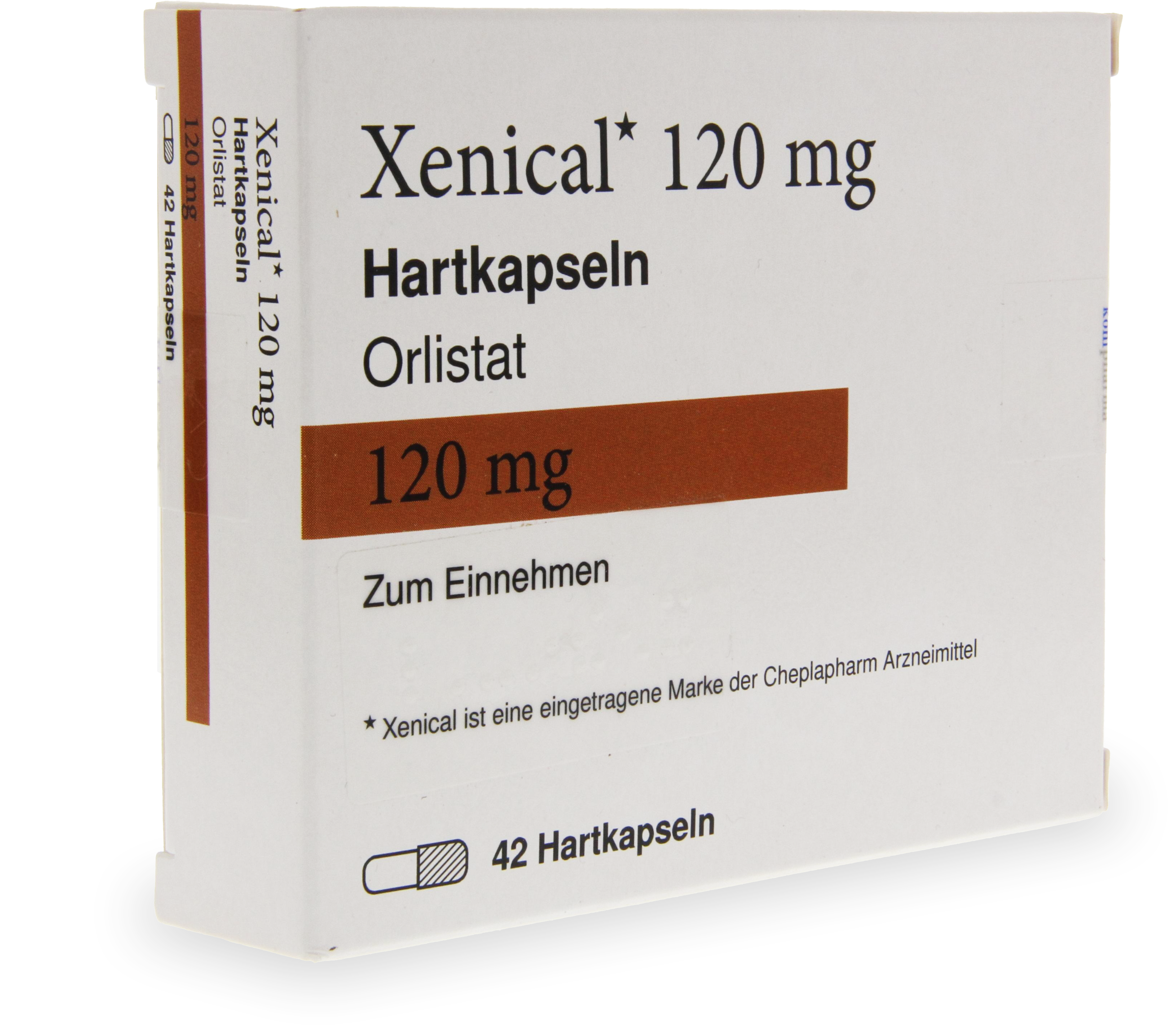
Orlistat blocks approximately 30% of dietary fat absorption and requires a reduced-fat meal plan
About Weight Loss
The Medical Case for Prescription Weight Loss
Obesity is recognised by the World Health Organization and NHS England as a chronic, relapsing disease driven by neurohormonal dysregulation, not simply excess calorie intake.
In the UK, 26% of adults are classified as obese (BMI 30+) and a further 38% as overweight, placing enormous strain on cardiovascular, metabolic, and musculoskeletal health.
When body weight increases, the hypothalamus recalibrates its "set point" and defends it vigorously.
Leptin resistance develops, ghrelin surges during calorie restriction, and adaptive thermogenesis reduces resting energy expenditure by 10-15%.
This explains why 80% of people who lose weight through dieting regain it within five years — the body actively fights to restore its previous mass.
Clinical consequences of untreated obesity are extensive:
- Type 2 diabetes risk increases 7-fold at BMI 35+
- Hypertension prevalence doubles compared with normal-weight adults
- Obstructive sleep apnoea affects 40% of individuals with BMI above 35
- Osteoarthritis of the knee develops 4-5 times more frequently
- Certain cancers (endometrial, colorectal, post-menopausal breast) show dose-dependent risk increases
A weight reduction of just 5-10% produces measurable improvements: systolic blood pressure drops by 5-8 mmHg, HbA1c falls by 5-10 mmol/mol in those with diabetes, and triglycerides decrease by 15-20%.
These benefits underpin the NICE recommendation that pharmacotherapy should be considered when lifestyle intervention alone has not achieved adequate results after 3-6 months.
Prescription weight-loss treatment is not a shortcut.
It corrects the biological disadvantage that makes sustained weight loss so difficult, allowing patients to achieve and maintain clinically meaningful reductions.
Available Prescription Treatments
Three main classes of weight-loss medication are prescribed in UK clinical practice, each acting through a distinct mechanism.
GLP-1 receptor agonists represent the most significant advance in obesity pharmacotherapy. Semaglutide (Wegovy) is administered as a once-weekly subcutaneous injection, titrated from 0.
25 mg to a maintenance dose of 2.4 mg over 16-20 weeks. The STEP 1 trial demonstrated a mean weight loss of 14.9% versus 2.4% with placebo at 68 weeks.
Liraglutide (Saxenda) requires daily injection at 3.0 mg and produces approximately 8% weight loss.
Both drugs work by activating GLP-1 receptors in the brain that regulate appetite and satiety, and by delaying gastric emptying.
Orlistat (Xenical, 120 mg three times daily with meals) inhibits pancreatic lipase in the gut, preventing absorption of roughly one-third of ingested dietary fat.
Average weight loss is 5-7% over 12 months. The unabsorbed fat causes gastrointestinal side effects — oily stools, flatulence, faecal urgency — which incentivise dietary compliance.
Naltrexone/bupropion (Mysimba) combines an opioid antagonist with a noradrenaline-dopamine reuptake inhibitor, targeting the hypothalamic appetite centre and the mesolimbic reward pathway.
Expected weight loss is 5-8% at one year.
Eligibility criteria follow NICE Technology Appraisal guidance:
- BMI 30+ (or 27.5+ for South Asian, Black African, and Black Caribbean ethnicities)
- BMI 27+ with at least one weight-related comorbidity (type 2 diabetes, hypertension, dyslipidaemia, OSA)
- Demonstrated engagement with dietary and physical activity modifications
Your prescriber will assess which medication suits your clinical profile, considering factors such as injection tolerance, existing medications, and cardiovascular history.
What the Clinical Evidence Shows
The evidence base for modern weight-loss pharmacotherapy is robust and continues to expand. Understanding the trial data helps set realistic expectations and supports informed treatment decisions.
The STEP programme (Semaglutide Treatment Effect in People with Obesity) comprises multiple phase 3 trials. STEP 1 enrolled 1,961 adults without diabetes and demonstrated 14.
9% mean weight loss at 68 weeks with semaglutide 2.4 mg weekly. STEP 2, which included patients with type 2 diabetes, showed 9.6% weight loss.
STEP 3 added intensive behavioural therapy and achieved 16.0%. Notably, 32% of STEP 1 participants lost 20% or more of their body weight.
The SCALE programme for liraglutide 3.0 mg reported 8.0% mean weight loss versus 2.6% with placebo over 56 weeks.
The effect was sustained over three years in an extension study, provided the medication was continued.
Cardiovascular outcomes are particularly encouraging. The SELECT trial demonstrated that semaglutide 2.
4 mg reduced major adverse cardiovascular events (heart attack, stroke, cardiovascular death) by 20% in overweight and obese adults with established cardiovascular disease.
This was a landmark finding, establishing that weight-loss pharmacotherapy delivers hard cardiovascular endpoint reduction.
Common side effects of GLP-1 agonists are primarily gastrointestinal:
- Nausea (reported by 40-45% during titration, resolving in most within 4-8 weeks)
- Vomiting (approximately 24%)
- Diarrhoea (30%)
- Constipation (24%)
Rare but serious risks include pancreatitis (incidence under 0.3%), gallbladder events (1.
6%), and a theoretical concern regarding medullary thyroid carcinoma based on animal data, though human evidence has not confirmed this risk.
Patients with a personal or family history of MEN2 or medullary thyroid cancer should not use GLP-1 agonists.
Building Habits That Sustain Weight Loss
Medication addresses the hormonal barrier to weight loss, but long-term success depends on embedding sustainable behavioural changes.
Clinical guidelines from NICE (CG189) and the British Obesity and Metabolic Surgery Society emphasise that pharmacotherapy should always accompany — not replace — dietary and physical activity interventions.
Dietary strategy matters more than calorie counting alone. A protein intake of 1.2-1.6 g per kg of body weight preserves lean mass during weight loss and enhances satiety.
Distributing protein across three meals (25-30 g per meal) maximises the thermic effect of food. Fibre intake of at least 30 g daily supports gut health and slows glucose absorption.
Practical dietary approaches with strong evidence include:
- Mediterranean diet: associated with 30% lower cardiovascular risk in the PREDIMED trial
- Time-restricted eating (16:8 pattern): modest additional benefit when combined with calorie control
- Reducing ultra-processed food intake, which currently accounts for 57% of UK adult calorie consumption
Physical activity prescription should be progressive.
Start with 150 minutes of moderate-intensity activity per week (brisk walking, cycling at conversational pace) and increase towards 250-300 minutes for weight-loss maintenance.
Resistance training 2-3 times weekly prevents the 25-30% lean mass loss that typically accompanies calorie restriction.
Sleep and stress management are frequently overlooked. Adults sleeping fewer than 6 hours per night have 27% higher obesity prevalence.
Cortisol elevation from chronic stress drives visceral fat accumulation and increases cravings for energy-dense foods.
Self-monitoring — regular weighing, food logging, and step tracking — is the single strongest predictor of long-term weight maintenance in the National Weight Control Registry data spanning over 10,000 successful maintainers.
Safety Considerations and Monitoring
Prescription weight-loss treatments require ongoing clinical supervision to ensure safety and optimal outcomes.
Your prescriber will establish a monitoring schedule tailored to the medication selected.
For GLP-1 agonists, baseline blood tests should include HbA1c (to detect undiagnosed diabetes or monitor existing diabetes), renal function, liver function, and lipid profile.
These are repeated at 3-month intervals during the first year. Patients with type 2 diabetes on insulin or sulfonylureas need dose adjustments as weight falls, because hypoglycaemia risk increases.
Contraindications for GLP-1 agonists include:
- Personal or family history of medullary thyroid carcinoma or MEN2 syndrome
- History of pancreatitis (relative contraindication requiring specialist review)
- Severe gastroparesis or inflammatory bowel disease
- Pregnancy or planned pregnancy (discontinue at least 2 months before conception for semaglutide)
For orlistat, fat-soluble vitamin levels (A, D, E, K) should be monitored, and supplementation is recommended.
Orlistat may reduce absorption of levothyroxine, warfarin, ciclosporin, and oral contraceptives, requiring dose separation or adjustment.
The MHRA has issued specific guidance regarding GLP-1 agonists and gallbladder disease.
Patients should report right upper quadrant pain promptly, as rapid weight loss increases gallstone formation risk. Ultrasound evaluation is indicated if symptoms develop.
Treatment duration follows NICE guidance: if a patient has not lost at least 5% of initial body weight after 12 weeks on the full maintenance dose, the medication should be discontinued and alternative options discussed.
This threshold ensures prescribing remains evidence-based and cost-effective.
All patients should have access to follow-up consultations to report side effects, discuss progress, and receive ongoing dietary and behavioural guidance.
Weight regain after discontinuation is common (approximately two-thirds of lost weight within one year), which is why some patients benefit from long-term or cyclical treatment strategies.
Frequently Asked Questions
How much weight can I expect to lose on Wegovy?
What is the difference between Ozempic and Wegovy?
Do I need to inject myself with GLP-1 medications?
Will I regain weight after stopping the medication?
Can I take weight-loss medication if I have type 2 diabetes?
Is Orlistat still worth considering given newer treatments?
Dr. Ross Elledge
Consultant Surgeon · Oral & Maxillofacial Surgery
Verified Healthcare Professional
The medical information on this site has been reviewed by Dr. Ross Elledge (GMC registered) and is provided for educational purposes. It does not replace a face-to-face consultation with your GP or specialist. Always follow the advice of your prescribing doctor and read the patient information leaflet supplied with your medication.