Asthma and COPD Inhalers Prescribed by UK Doctors
Asthma affects 5.4 million people in the UK and COPD a further 1.2 million diagnosed adults. As a GP managing these conditions daily, I follow the NICE/BTS stepwise approach to ensure every patient receives the right inhaler at the right step. Poorly controlled asthma accounts for 1,400 deaths annually in the UK — most are preventable with correct preventer adherence and a current written action plan.
NICE recommends low-dose ICS as step 2 therapy when SABA use exceeds twice weekly indicating uncontrolled asthma
COPD patients with FEV1 below 50% predicted benefit from LABA/ICS combination inhalers per GOLD guidelines
Salbutamol reliever inhaler use exceeding 3 canisters per year signals the need for preventer therapy review
Correct inhaler technique is essential — studies show 70-90% of patients use their device incorrectly
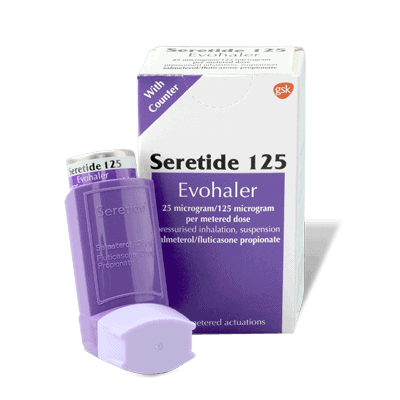
Seretide

Symbicort Turbuhaler
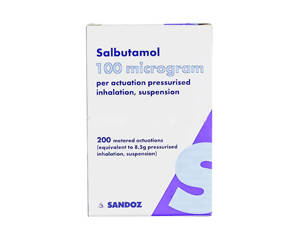
Salbutamol
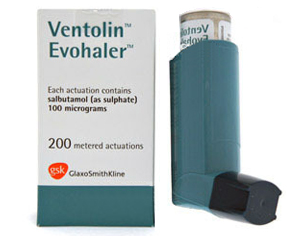
Ventolin

Bricanyl Turbohaler

Pulmicort Turbohaler
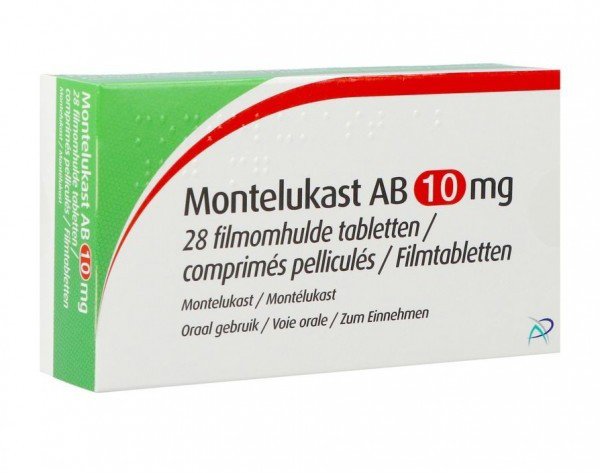
Montelukast
Flixotide
Serevent
Relvar Ellipta
Eklira Genuair
Onbrez Breezhaler
Spiriva

Anoro Ellipta

Atrovent
About Asthma & COPD
Understanding Asthma and COPD
Asthma and chronic obstructive pulmonary disease (COPD) are the two most common chronic respiratory conditions in the UK, sharing symptoms of breathlessness, wheeze, and cough but differing fundamentally in their pathophysiology and management.
Asthma is a chronic inflammatory airway disease characterised by reversible bronchoconstriction, airway hyper-responsiveness, and mucus overproduction.
Triggers include allergens (house dust mite, pollen, pet dander), exercise, cold air, respiratory infections, and occupational exposures. Peak flow variability exceeding 20% is a diagnostic hallmark.
In the UK, asthma affects approximately 1 in 11 children and 1 in 12 adults, with 5.4 million people currently receiving treatment.
COPD encompasses chronic bronchitis and emphysema, caused predominantly by tobacco smoke exposure.
It is characterised by progressive, largely irreversible airflow limitation confirmed by a post-bronchodilator FEV1/FVC ratio below 0.70 on spirometry. COPD affects an estimated 1.
2 million diagnosed individuals in the UK, though the true prevalence may be double this due to underdiagnosis.
Key differences between the conditions:
- Asthma onset typically before age 40; COPD usually after 40 with significant smoking history
- Asthma shows marked diurnal variation and trigger response; COPD symptoms are more persistent
- Asthma demonstrates significant bronchodilator reversibility (FEV1 improvement over 12% and 200 mL); COPD shows limited reversibility
- Eosinophilic inflammation predominates in asthma; neutrophilic inflammation in COPD
Some patients have features of both conditions, termed asthma-COPD overlap (ACO), occurring in approximately 15-20% of obstructive airways disease presentations.
These patients tend to have more frequent exacerbations and may require elements of both treatment pathways.
Both conditions carry serious consequences when poorly managed. Asthma causes approximately 1,400 deaths annually in the UK, the majority considered preventable.
COPD is the fifth leading cause of death in England and the second most common reason for emergency hospital admission.
Inhaler Types and the Stepwise Approach
The NICE and British Thoracic Society (BTS) guidelines use a stepwise approach to asthma management, escalating treatment until control is achieved and stepping down when stable.
COPD management follows the GOLD (Global Initiative for Chronic Obstructive Lung Disease) framework.
Step 1 — SABA reliever only: Short-acting beta-agonists such as salbutamol (Ventolin, Salamol) 100 mcg, 2 puffs as needed, provide rapid bronchodilation within 5 minutes, lasting 4-6 hours.
This step is appropriate only for patients with infrequent, intermittent symptoms. SABA use more than twice per week signals the need to step up.
Step 2 — Add low-dose ICS: Inhaled corticosteroids are the cornerstone of asthma prevention.
Beclometasone (Clenil) 200-400 mcg daily, budesonide (Pulmicort) 200-400 mcg daily, or fluticasone propionate (Flixotide) 100-250 mcg daily reduce airway inflammation, exacerbation frequency, and the risk of asthma death.
NICE now recommends a low-dose ICS/formoterol combination (MART regimen) as an alternative at this step.
Step 3 — Add LABA or increase ICS: Long-acting beta-agonists such as salmeterol or formoterol are added, usually as a combination inhaler (Seretide, Symbicort, Fostair).
LABAs must never be used without ICS in asthma due to increased mortality risk.
Step 4 — Medium/high-dose ICS + LABA: Increase ICS to medium or high dose within the combination inhaler.
Consider adding leukotriene receptor antagonist (montelukast 10 mg daily) or long-acting muscarinic antagonist (LAMA, e.g., tiotropium).
Step 5 — Specialist therapies: Referral for biologic therapies (omalizumab, mepolizumab, benralizumab) or oral corticosteroids under specialist supervision.
For COPD, the initial treatment depends on symptoms and exacerbation frequency:
- Group A (few symptoms, few exacerbations): SABA or SAMA as needed
- Group B (more symptoms): LABA or LAMA maintenance
- Group E (frequent exacerbations): LABA/LAMA combination; add ICS if blood eosinophils exceed 300 cells/mcL
Inhaler device selection matters as much as the drug. Metered-dose inhalers (MDIs) require coordinated inspiration, while dry powder inhalers (DPIs) are breath-actuated.
Spacer devices with MDIs improve lung deposition from approximately 10% to 20% and reduce oropharyngeal side effects.
Achieving and Maintaining Asthma Control
Asthma is considered well-controlled when a patient has minimal daytime symptoms (fewer than twice per week), no nocturnal waking, no limitation of daily activities, normal lung function, and uses their reliever inhaler no more than twice per week.
The Asthma Control Test (ACT) is a validated 5-item questionnaire that scores control from 5 (poorly controlled) to 25 (fully controlled), with a target of 20 or above.
Despite effective treatments being available, UK audit data reveals that asthma control remains suboptimal in approximately 45% of patients. The most common reasons are:
- Poor preventer adherence: Only 30-40% of patients take their ICS as prescribed. Electronic monitoring studies show that many patients use their preventer sporadically rather than daily, undermining its anti-inflammatory effect.
- Incorrect inhaler technique: Studies consistently show that 70-90% of patients make at least one critical error when using their inhaler device. Common mistakes include failing to shake an MDI, not exhaling fully before inhalation, and inhaling too rapidly with a DPI.
- Unidentified triggers: Allergen exposure (dust mites, mould, pet dander), occupational sensitisers, and gastro-oesophageal reflux contribute to ongoing symptoms.
Self-management strategies supported by NICE guidance include:
- Written personalised asthma action plan — reduces hospitalisation risk by 30-40%
- Peak flow monitoring: measure morning and evening PEF; a fall below 80% of personal best indicates worsening control
- Recognise early warning signs: increasing reliever use, nocturnal cough, reduced exercise tolerance
- Annual influenza vaccination and pneumococcal vaccination where eligible
Environmental control measures:
- Allergen-proof mattress and pillow covers to reduce dust mite exposure
- Maintain indoor humidity below 50% to inhibit mould growth
- Avoid known triggers including tobacco smoke, strong perfumes, and cold dry air
- Consider occupational health referral if symptoms worsen at work
Regular clinical review (at least annually) includes spirometry, inhaler technique assessment, medication adherence check, and formal asthma control assessment.
Patients using 3 or more SABA canisters per year require urgent preventer therapy review.
COPD Management and Exacerbation Prevention
COPD management aims to reduce symptoms, improve exercise capacity, and prevent exacerbations.
Unlike asthma, airflow limitation in COPD is not fully reversible, but effective pharmacotherapy significantly improves quality of life and reduces hospital admissions.
Smoking cessation is the single most important intervention, slowing the accelerated decline in FEV1 from approximately 60 mL/year to the normal age-related rate of 25-30 mL/year.
Varenicline (Champix), nicotine replacement therapy, and behavioural support are available through NHS Stop Smoking Services, with quit rates of 25-30% at 12 months.
Pharmacological management follows GOLD guidelines:
- SABA (salbutamol) or SAMA (ipratropium) for immediate relief
- LABA (formoterol, salmeterol, indacaterol) for persistent breathlessness
- LAMA (tiotropium, glycopyrronium, umeclidinium) — the most effective single bronchodilator class in COPD, reducing exacerbations by 20-25%
- LABA/LAMA combinations (Ultibro, Anoro, Spiolto) for patients with persistent symptoms on monotherapy
- Triple therapy (ICS/LABA/LAMA — Trelegy, Trimbow) for patients with frequent exacerbations and blood eosinophils above 100 cells/mcL
ICS use in COPD is more restricted than in asthma. NICE recommends adding ICS only when exacerbations persist despite dual bronchodilator therapy and blood eosinophils are elevated.
Inappropriate ICS use in COPD increases pneumonia risk by 30-50%.
Pulmonary rehabilitation is an evidence-based exercise and education programme lasting 6-8 weeks.
Cochrane review data shows it improves breathlessness, exercise capacity, and health-related quality of life more effectively than any single medication.
All patients with MRC dyspnoea grade 3 or above should be referred.
Exacerbation management:
- Rescue pack: prednisolone 30 mg daily for 5 days plus a standby antibiotic (amoxicillin or doxycycline)
- 2-3 exacerbations per year warrants review of maintenance inhaler therapy
- Post-exacerbation follow-up within 2 weeks to assess recovery and adjust treatment
Oxygen therapy (LTOT, long-term oxygen therapy for at least 15 hours daily) is indicated when resting PaO2 falls below 7.3 kPa on stable blood gas assessment.
Ambulatory oxygen benefits patients who desaturate on exercise.
Ordering Inhalers Through Dr. Presc
Repeat inhaler prescriptions can be obtained through Dr. Presc following a clinical assessment that mirrors the standards expected in NHS primary care.
The process is designed for patients with an established respiratory diagnosis who need convenient access to their maintenance inhalers.
The consultation assesses:
- Current diagnosis and severity classification
- Inhaler history: which devices and doses you currently use
- Symptom control: frequency of reliever use, nocturnal symptoms, activity limitation
- Exacerbation history: oral steroid courses or emergency department visits in the past 12 months
- Smoking status and exposure history
- Adherence patterns and inhaler technique confidence
Prescribing standards we follow:
- SABA reliever inhalers are prescribed alongside preventer therapy, never as sole treatment for persistent asthma
- ICS dose is matched to current control level following NICE/BTS step guidelines
- COPD inhaler selection aligns with the GOLD ABCD assessment framework
- Patients requesting excessive SABA quantities are counselled and referred for asthma review
Safety checks include:
- Screening for oral candidiasis risk with ICS (advise mouth rinsing after each dose)
- Identifying patients on beta-blockers who require cardioselective agents only
- Flagging LABA monotherapy requests in asthma patients (contraindicated without ICS)
- Verifying influenza and pneumococcal vaccination status
All prescriptions are dispensed by GPhC-registered pharmacies.
We offer the full range of branded and generic inhaler devices, and our prescribers can switch between equivalent devices if your preferred brand is unavailable.
Important limitations: New respiratory diagnoses require face-to-face assessment including spirometry, which cannot be performed remotely.
Patients experiencing acute exacerbations with severe breathlessness, cyanosis, or confusion should attend A&E immediately rather than seeking an online consultation. Dr.
Presc is designed for maintenance therapy management, not acute care.
Annual review with your NHS GP or practice nurse remains recommended alongside online prescribing, to ensure spirometry is performed, inhaler technique is observed, and your written action plan is updated.
Frequently Asked Questions
How often should I use my preventer inhaler?
When should I use my blue reliever inhaler?
What is a MART regimen?
Can I get asthma inhalers without a diagnosis?
Do inhaled corticosteroids cause long-term side effects?
What is the difference between a LABA and a LAMA?
Dr. Ross Elledge
Consultant Surgeon · Oral & Maxillofacial Surgery
Verified Healthcare Professional
The medical information on this site has been reviewed by Dr. Ross Elledge (GMC registered) and is provided for educational purposes. It does not replace a face-to-face consultation with your GP or specialist. Always follow the advice of your prescribing doctor and read the patient information leaflet supplied with your medication.
